-

Premenstrual Dysmorphic Disorder/Premenstrual Syndrome Luteal Phase Treatment
Shelby Gawarecki
• PMS/PMDD symptoms affect many women's emotional and physical wellbeing.
• SSRIs, progesterone, and sepranolone are luteal phase treatment options.
• Studies were all peer-reviewed, including randomized control trials or a meta-analysis.
• SSRIs are a consistent primary treatment for symptom alleviation especially cognitive symptoms. SSRIs are the current mainstay, recommended for luteal phase treatment of PMS/PMDD.
• SSRIs, including citalopram, sertraline, escitalopram, and fluoxetine, were examined to determine their efficacy in relieving mood-related symptoms such as irritability, anxiety, and depression during the luteal phase.
• Data on progesterone treatment in the luteal phase is inconclusive. • Allopregnanolone levels and sepranolone treatment research are currently delivering a new understanding of hormonal mechanisms in PMS/PMDD.
• Sepranolone remains in trial and is not yet available for clinical use.
-
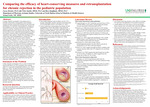
Comparing the Efficacy of Heart-Conserving Measures and Retransplantation for Chronic Rejection in the Pediatric Population
Lacey Zeiszler
Coronary allograft vasculopathy is the leading cause of morbidity and mortality among pediatric heart transplant recipients and faces unsuccessful treatment for prevention and management. Post-transplant immunosuppressive therapy has been modified over the years to determine the most effective regimen for rejection. Tacrolimus has been the superior immunosuppressant used for rejection since the early 2000s. It has been shown to have substantial immunosuppressive effects, least number of adverse effects, and decreased comorbidities compared to other regimens. Despite these advantages, CAV is still prevalent. Heart retransplantation is currently the only curative treatment. We used Google Scholar, PubMed, ClinicalKey, ScienceDirect, Elsevier, Wiley Online Library, and National Library of Medicine to compare current data on heartconserving measures and heart retransplantation for CAV in the pediatric population. New drugs have become available that bear comparison with tacrolimus, such as everolimus (EVL) and sirolimus. These drugs are shown to be more effective in preventing and managing CAV than tacrolimus long-term. Incorporating widely known drugs, such as statins and aspirin, into regimens have been observed to have no effect on chronic rejection. Advanced technology has produced drug-eluting stents small enough for pediatric patients for short-term use as restenosis is inevitable. Heart retransplantation is inferior to heart-conserving measures as complications decrease life expectancy significantly more.
-

Minimally Invasive Therapies in the Treatment of Arthropathy
Steven Bateman
This literature review explores the efficacy of minimally invasive therapies that precede and delay surgical intervention in adult patients experiencing functional limitations and pain in major joints. The effectiveness of physical therapy and injections such as corticosteroids, hyaluronic acid, platelet-rich plasma, and mesenchymal stem cells (MSC) was evaluated. A comprehensive search of PubMed utilizing MeSH terms yielded 114 relevant studies, which were screened based on inclusion criteria of human studies published within the past five years. Keywords included mesenchymal stem cells, stem cells, mesenchymal, arthroplasty, and joints. Producing few results, inclusion criteria were later expanded to include studies within the past ten years, their references, articles citing results, and articles similar to results. Of note, the chondrotoxic nature of corticosteroid (CS) injections suggests alternative first-line therapies in hyaluronic acid (HA) and platelet-rich plasma (PRP), particularly in earlier stages of disease. Regarding MSC findings, low side-effect profiles with evidence of induced regeneration are encouraging, but studies that evaluate their effectiveness compared to other treatments are lacking. Although MSC therapies lack a robust evidence base, their potential warrants further investigation.
-

Does Supplementation with Vitamin D and Calcium Reduce the Risk of Developing Pre-eclampsia Compared with Prophylactic Daily Aspirin Use?
Katja Berge
Pre-eclampsia is a hypertensive disorder that occurs during pregnancy. Onset is typically around the 20 week of gestation and serious complications may occur if it is not properly managed. Complications from pre-eclampsia include preterm delivery, disease progression to eclampsia, organ damage, placental abruption, and neonatal complications. Initial management involves the use of antihypertensive medications. Current guidelines recommend the initiation of 81 mg aspirin starting at 12 weeks gestation for women with increased risk factors. The goal of this literature review is to examine the effectiveness of calcium and vitamin D supplementation compared to daily prophylactic aspirin use for prevention of pre-eclampsia. The databases utilized for this literature review include Pub-Med, Cochrane Library, Clinical Key, and Google Scholar. Additional relevant studies were found in reference lists of the included studies. This comprehensive review will discuss initiation of therapy, dosing, and pregnancy outcomes. Review of the literature showed a decrease in blood pressure with the use of calcium and vitamin D supplementation. However, there was a greater impact shown with calcium supplementation in populations with a dietary deficiency than those without a dietary deficiency in calcium. The effect of 150 mg daily prophylactic aspirin was shown to reduce the occurrence of preterm pre-eclampsia but did not impact preeclampsia after 37 weeks of gestation.
-

Treating Rheumatoid Arthritis: Immunosuppression Versus Stem Cell Therapy
Bailee Blickensderfer
This literature review will discuss the difference in efficacy and side effect profile between methotrexate monotherapy and mesenchymal stem cell therapy for the treatment of rheumatoid arthritis. Rheumatoid arthritis is a debilitating inflammatory condition that effects a person’s mobility and can cause chronic, intense pain. Due to the side effect profile of methotrexate, mesenchymal stem cell therapy is being investigated as a treatment option. There were 11 scholarly articles evaluated for the purpose of this literature review. Data compiled from these studies supports the use of Mesenchymal stem cells as treatment for rheumatoid arthritis due to immunomodulatory effect on multiple immune components that contribute to the development of rheumatoid arthritis. Mesenchymal stem cell treatment was also less likely to cause serious side effects than methotrexate therapy. However, the determination of whether mesenchymal stem cell therapy is definitively more effective than methotrexate monotherapy cannot be made. This is due to a lack of robust research available for the evaluation of mesenchymal stem cell therapy on rheumatoid arthritis. Additionally, the exact mechanism by which mesenchymal stem cells provide the desired immunomodulatory effects is not yet well understood.
-
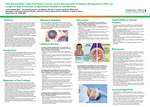
Viral Bronchiolitis: High Flow Nasal Cannula versus Non-Invasive Ventilation Management’s Effect on Length of Stay, Prevention of Mechanical Ventilation, and Mortality
Justis Caldwell
• This research aimed to review the literature relating to pediatric patients hospitalized with viral bronchiolitis and determine if there is a difference between high-flow nasal cannula (HFNC) and non-invasive ventilation (NIV) in preventing mechanical ventilation, decreasing the length of hospital stay, and decreasing morbidity and mortality.
• A literature review was performed using the electronic search database PubMed. Keyword and mesh terms were used to define a set of literature discussing the use of high-flow nasal cannula versus continuous positive airway pressure in the management of viral bronchitis in pediatric patients. The search revealed a total of 37 studies. All searches were narrowed down to the last five years. Studies that included nebulized, pharmacological treatments were excluded. There were ten studies that met the final criteria.
• The literature suggests that the use of CPAP for initial treatment had better success in not escalating support, but patients on CPAP typically had a longer length of stay. This could have been because if the patient had to be on CPAP, then they had more severe bronchiolitis. There is also the factor of the patient's discomfort with using CPAP. This could cause the need for some sedation to make them more comfortable with the device and also a need for weaning off the sedation. There was no difference in the intubation rate between the two support modes.
-

Mobilized Healthcare: the Future of Accessible Medicine
Zachary Carlson
This paper discusses the impact that Mobile Integrated Healthcare teams can have in our health system. It is well known that there are communities that benefit from MIH teams such as rural or underserved areas; however, this paper discusses a variety of other demographics that may benefit from implementation of MIH teams. It will also evaluate how MIH teams alter patient Emergency Department (ED) visits, hospital admissions, facility spending, and patient outcomes. MIH is a form of preventative medicine that may be better optimized by healthcare facilities going forward, and this article helps to weigh the pros versus cons of MIH team implementation in local communities. This article demonstrates how MIH teams can help reduce overall hospital and ED admissions as well as decrease hospital spending and show patient outcome improvement overall. These findings further support the concept of communities initiating MIH teams more abundantly.
-

Efficacy of Vitamin D versus Biological Agents in the Management of Rheumatoid Arthritis
Kayli Day
Rheumatoid arthritis (RA) is a chronic inflammatory disease leading to joint destruction. There are several treatment options available to patients, including conventional disease modifying antirheumatic drugs (DMARDS) and biological agents, but their efficacies vary per patient and tote significant adverse effects and cost. There is, however, encouraging evidence to suggest the incorporation of vitamin D in treatment regimens may be a promising option for patients. A comprehensive literature review was conducted using PubMed and CINHAL databases, employing keywords and MeSH terms related to RA treatment options, with the goal to compare efficacy of biological agents and vitamin D in the symptom management and progression of RA. Eleven studies met criteria and were analyzed. These studies evaluated vitamin D, tumor necrosis factors, interleukin inhibitors, B-cell inhibitors, and T-cell inhibitors in the treatment and prevention of RA progression. The review highlights the complexity of managing RA and underscores the favorable outcomes observed in symptom management and disease progression by biological agents compared to vitamin D. Although vitamin D demonstrates promise as an adjunctive and potential preventative therapy, further research that includes vitamin D as part of a treatment regimen with biologics is necessary to evaluate its potential and proper use in the treatment of RA. Providers must remain informed about optimal practice recommendations, be amenable to a trial-and-error approach to treatment, and consider combination therapy, with use of DMARDS, biologics, and adjunctive therapies such as vitamin D to best meet the needs of individual patients.
-

Sebaceous Carcinoma: A Commitment to a Standard of Care
Stephany Janice Sophia Dimoulas
Sebaceous carcinoma (SC) has its origin in the sebaceous glands of the dermis and may develop as a result of de novo mutations from benign sebaceous neoplasms or as a result of microsatellite instability and loss of mismatch repair gene expression secondary to Muir-Torre Syndrome (MTS). SCs may also arise from the Meibomian glands, the glands of Zeis, or the sebaceous glands of the caruncle if occurring periocularly. Although SCs may occur at any sebaceous gland-containing location, the most common areas of involvement include the periocular, head, and neck regions. Given its capacity for nodal and distal metastasis as well as its association with significant morbidity and mortality, surgical excision must be pursued. The high recurrence rate and tendency of misdiagnosis that are associated with SCs, warrant swift diagnostic measures and the establishment of a gold-standard method of surgical treatment. Therefore, the purpose of this literature review is to compare the efficacies of MMS and WLE in the prevention of recurrence and metastasis of both extraocular and ocular SCs.
-

Blood Based Multi-Cancer Early Detection Tests in Lung Cancer Screening
Maren Dockter
Lung cancer is responsible for the most cancer-related deaths worldwide. While the implementation of low dose CT (LDCT) screening for high-risk individuals has been shown to improve outcomes and reduce mortality by 20%, there is still room for improvement in screening (de Koning et al, 2020). Multi-cancer early detection (MCED) tests aim to detect early-stage cancer with the goal of improving treatment outcomes. This technology combines plasma analysis for cell-free DNA and methylation patterns with artificial intelligence to detect malignancies and predict tumor origin sites. The purpose of this systemic literature review is to assess the rising potential of MCED for screening and early detection of lung cancer compared to LDCT. This review utilizes searches of PubMed and ClinicalKey. A total of 14 articles published over the last 20 years were included for analysis. Results indicate that MCED has a higher specificity than LDCT resulting in less false positives, however, the sensitivity of MCED for detecting lung cancer is not consistently high enough to replace LDCT. At this time, LDCT remains the gold standard for screening and early detection of lung cancer and should continue to be utilized in clinical practice. This study focused exclusively on lung cancer, but MCED has the capability to detect more than 50 types of cancer, many without a current screening. Further research should be conducted to explore the role of MCED as an adjunct to traditional cancer screenings.
-

Let’s Move! Benefits of Exercise Compared to SSRIs (escitalopram) for the Management of Depression: Research from 2020 and Beyond
Brianna Droessler-Aschliman
• Purpose: Determine the effectiveness of exercise as either monotherapy or in combination with SSRIs (selective serotonin reuptake inhibitors) for the management of major depressive disorder.
• Studies gathered for this review came from the following databases: PubMed, SpringerLink, Academic Search Ultimate, Academic Search Complete, and CINAHL.
• Review of current research that was completed between the years 2020-2023 that consisted of either clinical trials, RCTs, or meta-analysis. • Upon completion of the literature review: exercise is equivocal to SSRIs as a treatment option. While this is a significant finding, the benefits of exercises are more consistent in those that adhere to a program and are more effective if prescribed in combination with SSRIs.
• It would require providers to have the knowledge and awareness of appropriate exercise modalities and resources available to the patients. It is also vital that providers offer support to patients and encourage compliance with their programs.
-

Lifestyle Changes and Medication vs. Medication Alone: Symptom Control of Parkinson Disease
Rachel Duncan
Parkinson disease is multifactorial and predominantly effects the geriatric population. The mainstay of treatment for patients diagnosed is currently symptomatic treatment with dopamine replacement. The goal of this literature review is to identify possible lifestyle modifications that can delay progression of the disease or help prolong OFF time of symptoms. Lifestyle modification predominantly considered during this review included diet and physical activity. Included in the study were MIND, Mediterranean, and DASH diets. Considering the role of medication in this disease levodopa, dopamine agonists, monoamine oxidase B inhibitors and the addition of ropinirole to levodopa and their efficacy in treating parkinsonian symptoms was investigated. A literature review was conducted using electronic search database including, PubMed, Clinical Key and DynaMed. After thorough review of 12 articles regarding management of Parkinson disease with various modifications along with medications it was found lifestyle modifications are not significant in the management of Parkinson disease alone. However, there is evidence to support the benefits lifestyle modifications can have, including diet and physical activity, for those diagnosed with Parkinson disease. The addition of these changes have shown the possibility of reducing the OFF time in the disease as well as reducing the daily medication regimen needed.
-

Comparing Effectiveness of Intrauterine Devices Versus Oral Contraceptives for Management of Dysmenorrhea
Mackenzie Holland
The purpose of this research and systematic literature review is to determine if oral contraceptives or intrauterine devices are more effective in the treatment of dysmenorrhea pain. It is estimated that at least 50% of women worldwide live with dysmenorrhea and there is very little research determining what the best treatment options are for it. The main treatment recommended by health care providers for dysmenorrhea are non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen. However, this treatment option may not provide the relief that women with this condition need. This review used three main databases, including PubMed, Embase, and Clinical Key in order to find pertinent research and articles. A variety of key words were used in the search, such as dysmenorrhea, oral contraceptives, and intrauterine devices. The studies found were then narrowed down by excluding studies older than 2011 and including relatively pertinent studies that were either randomized controlled trials, clinical trials, open-label, parallel group studies, interventional studies, observational studies, secondary analyses, or pilot studies. Out of the studies included in this review, only one compared the effectiveness of oral contraceptives and intrauterine devices. Each study reviewed showed that oral contraceptives and intrauterine devices were safe and effective options, but in the single head-tohead study, it was determined that intrauterine devices were superior. The evidence also showed that intrauterine devices were often not as well tolerated and resulted in discontinuation of use due to the side effects. Despite the results of the article, more research needs to be conducted prior to making a definitive decision on the best treatment method for dysmenorrhea pain.
-

Treatment of Irritable Bowel Syndrome: Tricyclic Antidepressants vs. Diet Modification and Visceral Manipulation
Alexis Int Veldt
• Introduction: The purpose of this study analysis is to compare tricyclic antidepressant (TCA) to diet modification and visceral manipulation in the treatment of irritable bowel syndrome (IBS).
• Research Methods: Three databases were searched including PubMed, Google Scholar and ClinicalKey, within a time frame of 20 years. Studies chosen for review were peer reviewed and focused on randomized control trials.
• Discussion:
– Diet modification appears to be the most beneficial with the least amount of side effects when compared to TCA use, however, more research needs to be done to evaluate how patients react to reintroduction of foods with elimination diets.
– Visceral manipulation appears to help with refractory symptoms, but more studies need to be conducted due to the newer usage of this option as a treatment for IBS.
– Tricyclic antidepressants are currently one of the most effective medications for overall symptom improvement, however, more side effects are seen with this treatment option due to anticholinergic effects of these medications.
– Due to the multifactorial process of IBS, a combination of treatment options is likely to benefit patients more than a single approach alone, to adequately treat patient symptoms.
-

Efficacy of Platelet Rich Plasma Injections to Combat Chronic Tendinopathies
Rachel Kisse
➢ Tendinopathy is a clinical syndrome marked by persistent localized pain and tendon thickening, stemming from repetitive overuse. It poses diagnostic and management challenges due to its chronic nature..
➢ This literature review was performed to inform clinicians about the properties, safety, and efficacy of PRP injections as an adjunctive therapy in chronic tendinopathies, specifically the epicondylar and Achilles tendons. A comprehensive review of 12 clinical trials, exploring the efficacy of PRP injections was performed. The primary focus of this review looked into the trends in efficacy, including pain reduction and activity improvement, using various functional assessment scales like the VAS, PRTEE, DASH and VISA-A.
➢ Overall, studies comparing PRP with various modalities show promise in reducing pain, improving function, and fostering tendon regeneration. Combining PRP with physical therapy often yields superior outcomes, urging further exploration of optimal PRP formulations, concentrations, injection intervals, and the role of ultrasound guidance. Addressing current limitations and optimizing protocols through further research will enhance our understanding and utilization of PRP in tendinopathy treatment.
-

Comparison of Platelet-Rich Plasma Injections and Hyaluronic Acid Injections in the Treatment of Knee Osteoarthritis
Isaac Knutson
Osteoarthritis is one of the most common diseases that people can suffer from in today’s society. This degenerative disease can affect any of the body’s joints, but is most common in the knees, hands and spine. This review studied the effects of two specific treatments for knee osteoarthritis: platelet-rich plasma injections and hyaluronic acid injections. Both of these treatments can be provided by a primary care provider that has the proper training as well as an orthopedic specialist. Platelet-rich plasma injections (PRP) are the patient’s own blood products reintroduced into the affected joint to stimulate healing. Hyaluronic acid (HA) occurs naturally in the body, and when injected into a joint suffering from osteoarthritis, it can act as a joint lubricator/shock absorber to help decrease pain and improve function. The results of this study show that both platelet-rich plasma and hyaluronic acid injections can be effective in the treatment of knee osteoarthritis. However, platelet-rich plasma was shown to be more effective in reducing pain, increasing range of motion, and improving overall function.
-

The Efficacy of GLP-1 Agonists in Pediatrics with Type 2 Diabetes and Obesity
Cayla Mahrer
GLP-1 therapies show promise in managing type 2 diabetes and obesity in adolescents. This review explores the efficacy, safety, and variations in treatment outcomes. GLP-1 therapies (liraglutide, dulaglutide, exenatide) effectively reduce HbA1c levels. Weight reduction is a positive outcome crucial for type 2 diabetes and obesity management. Safety concerns and gastrointestinal effects emphasize the need for monitoring during GLP-1 therapy. Insights from studies on Lixisenatide offer valuable information for healthcare providers. There is consensus on general effectiveness, but debates on specific outcomes and long-term effects persist. Case-based investigations suggest potential variations in treatment responses, requiring further exploration. Bridging the gap between research and application. Empowering clinicians to make informed decisions, considering individual patient needs for enhanced quality of care.
-
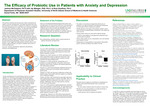
The Efficacy of Probiotic Use in Patients with Anxiety and Depression
JoAnna McClelland
The gut-brain connection has become more widely researched for its impacts on anxiety and depression. This bodes the question that if the gut microbiome can be altered, would there be a decrease in symptoms of anxiety and depression as a result? One way to alter gut microbiome is to implement a prebiotic or probiotic. To determine if this is an effective treatment option for anxiety and depression, a literature review was conducted using primarily randomized clinical trials. PubMed was the primary database that was used for this research. Articles were sorted and chosen based upon applicability to the problem being investigated, clinical trials, and a recent time frame of five years. Most of the articles reviewed found statistically significant differences in improvements of symptoms of anxiety and depression in the intervention group participants. Therefore, the results of this literature review suggest that implementing a probiotic either as sole therapy or adjuvant therapy can improve symptoms and severity of anxiety and depression.
-

Comparison of Cryopreservation of Ovarian Tissue Versus Cryopreservation of Oocytes in Fertility Preservation
Madison Nitschke
This literature review aims to compare ovarian tissue cryopreservation (OTC) and oocyte cryopreservation (OC) as methods for fertility preservation. Electronic health science databases including PubMed, Clinical Key, ScienceDirect, and UpToDate were utilized. Seven articles met the inclusion criteria and were analyzed for this comprehensive review. This review indicates that both oocyte and ovarian tissue cryopreservation can effectively preserve fertility, however, ovarian tissue cryopreservation is deemed most effective for prepubertal girls at high risk of iatrogenic primary ovarian insufficiency (POI), or women who are unable to postpone gonadotoxic treatment. Ovarian tissue cryopreservation offers advantages that oocyte cryopreservation does not, such as multiple spontaneous pregnancies and resumption of ovarian function. Ovarian tissue cryopreservation also does not carry the risks associated with ovarian stimulation and delaying gonadotoxic treatment, unlike oocyte cryopreservation. Despite successful birth rates and low surgical risks associated with ovarian tissue cryopreservation, studies reveal a low utilization rate, with women often considering stored ovarian tissue as a “backup plan”. There is a need for further additional research on ovarian tissue cryopreservation, especially in the younger age groups, as there was limited participation in follow-up studies. Overall, the studies analyzed in this literature review support ovarian tissue cryopreservation as an effective method of fertility preservation but emphasize the importance of further investigation and follow-up studies.
-

Patient Outcomes With Tele-Emergency Medicine Services in Rural Areas
Andrea Rieder
The purpose of this literature review was to examine patient outcomes with the use of tele-emergency medicine. Teleemergency medicine serves as a tool to expand the healthcare team in rural facilities by connecting them with specialized providers, typically via video conference call, for assistance in surge or lowstaff situations, or for guidance in more complicated cases that rural providers might typically transfer to a larger hospital. A benefit of adopting a tele-emergency medicine service is that it can shorten time to care and reduce the need for transfers, thereby reducing associated costs. The question arises as to whether patient outcomes are improved as well, or if the limitations of telemedicine lead to lower quality of care. For this review , databases such as PubMed and Embase were used to compile current research on the topic. The results of this study suggest that the quality of patient care does seem to improve with the use of tele-emergency medicine. This is demonstrated by measures such as a decrease in medical errors and positive reviews from medical staff. Discharge status appeared to be affected by using teleemergency medicine, resulting in increased admissions, decreased discharges, and decreased transfers.
-

Probiotic Therapy for the Treatment and Prevention of Bacterial Vaginosis
Chelsea Scheil
Bacterial vaginosis (BV) is a common presenting complaint in healthcare, and patients often experience recurrences at a frustrating rate. The mainstay of current treatment is antibiotic therapy, either via oral or vaginal route. When recurrences occur, stronger antibiotics are often employed. This current method of treatment does not address an underlying component that impacts infection recurrence and rate of recurrence- the patient’s baseline vaginal microbiome and the healthy bacteria that support it. To investigate the use of probiotics in bacterial vaginosis treatment, a comprehensive literature review was completed using databases PubMed and Embase. The results of this literature review confirm that probiotic therapy is safe for the treatment of BV. There are a variety of different probiotic bacterial strains and concentrations utilized for either monotherapy to treat BV or in conjunction with antibiotic therapy. Of the bacterial strains analyzed, those that were most studied were L. crispatus and L.rhamnosus via both oral and vaginal use. Both oral route and vaginal route of probiotic treatment were shown to be effective. Vaginal route showed a faster impact on microbiome, but also a faster rate of recurrence than oral probiotic use. Probiotic therapy alone or in conjunction with antibiotics was found to be more effective than placebo or the use of only antibiotics to treat BV. Further research is still needed regarding identifying all possible bacterial strains that are beneficial in treating/preventing BV, differing combinations of strains for increasing efficacy, along with identifying the necessary concentrations of these strains.
-

SSRI/SNRI Medication vs. Cognitive Behavioral Therapy in the Treatment and Management of Postpartum Anxiety
Kelsey Sederquest
The purpose of this literature review is to determine the effects of cognitive behavioral therapy (CBT) and Selective Serotonin Reuptake Inhibitors/Selective Norepinephrine Reuptake Inhibitors (SSRI/SNRI) in women suffering from postpartum anxiety. Efficacy of non-pharmacological, pharmacological, and combination therapy compared within this review. Lastly, prophylactic treatment of anxiety was examined in women who were pregnant or who were newly postpartum without diagnosis of anxiety. In this review the database PubMed was utilized to conduct research that included many different keywords. The articles included were limited to within the last 30 years, and research was narrowed by limiting patient population to postpartum women and eliminating articles that did not evaluate CBT or SSRI/SNRI medication as a form of treatment for anxiety during the postpartum period. The data presented shows evidence that CBT and SSRI/SNRI pharmacological treatment are effective in the treatment of postpartum anxiety, which indication that CBT is more effective in the short term, while pharmacological treatment may be more beneficial for patients needing long term treatment. Analysis of literature did not show any evidence suggesting statistically more significant reduction or remission of symptoms when combining non-pharmacological and pharmacological treatments. Further research should be conducted to explore potential benefits of prophylactic treatment in the antepartum period for postpartum anxiety.
-

Exercise and Preventing Dementia in Older Adults
Valerie Snelling
Dementia is a devastating diagnosis for millions of individuals and the prevalence is projected to increase significantly in the next 30 years. According to the Centers for Disease Control and Prevention (2019), there are over five million individuals aged 65 and over living in the United States with dementia. That number is estimated to increase to 14 million by 2060. The impact of the increasing prevalence of dementia is significant. Because dementia is a complex disease caused by over 50 underlying health conditions, finding effective treatments for the disease is difficult. This makes prevention of dementia extremely important. The purpose of this literature review is to analyze if exercise prevents dementia in older adults. Studies were included if they analyzed physical activity with the onset of dementia or changes in various cognitive abilities. This literature available to date indicates that exercise is an effective measure to prevent dementia in older adults.
-

Exercise Effect on Gestational Weight Gain and Diabetes in Women of Elevated BMI
Lauren Staton
The purpose of this literature review is to determine the effect of exercise on gestational weight gain and diagnosis of gestational diabetes. Maternal obesity is a risk factor that may increase the likelihood of adverse outcomes during pregnancy such as excessive weight gain, gestational diabetes, macrosomia, and cesarean delivery. As obesity has become a more prevalent diagnosis, the healthcare field is beginning to see its effects on an abundance of patient profiles, including pregnant women. In the primary care setting, providers are the source of information for patients as to what healthy weight gain during pregnancy looks like. By implementing recommendations for exercise throughout gestation, excessive weight gain and its associated adverse outcomes may decrease in frequency. This literature review examines the efficacy of prescribed exercise programs on the abovementioned outcomes. Research databases including PubMed and ClinicalKey were used to find studies looking at the effect of exercise on weight gain and diabetes diagnosis during pregnancy. Inclusion and exclusion criteria, later discussed in the methods section, were used to further narrow down papers. Results of this study showed that exercise was able to decrease occurrence of excessive weight gain and gestational diabetes diagnosis in women with pre-pregnancy BMIs in the overweight and obese categories. Further research may need to be done that evaluates the role of physical activity in addition to nutrition, as both are key components to gaining healthy weight during pregnancy.
-

Effects of Probiotic Supplementation on PCOS Outcomes
Allison Stoeffler
Polycystic ovarian syndrome (PCOS) is a multifactorial metabolic, endocrinologic, and gynecologic condition affecting up to 5 million women in the United States. It is a disease characterized by oligo- or anovulation, hyperandrogenism, and/or polycystic ovaries. Phenotypic presentation can include irregular menstrual cycles, obesity, hirsutism, insulin resistance, or difficulty conceiving. If untreated, PCOS can result in a sequelae of chronic disease burden. Current standard of care consists of metformin for blood sugar control, oral contraceptives for menstrual regularity, and spironolactone for androgen imbalance, but newer research is identifying gut dysbiosis as a possible contributing etiology to disease development and symptomology. This literature review aims to investigate the effectiveness of probiotic supplement regimens in improving the gut microbiome and subsequent outcomes for patients with PCOS, specifically inflammatory, anthropometric, androgen, and blood sugar markers. A comprehensive literature review was performed using PubMed and Clinical Key databases. A variety of keywords and similar articles were used to identify studies that were further screened for inclusion and exclusion criteria. Studies were excluded if they were systematic reviews, published over 10 years ago, utilized non-human subjects, had poor study design, or looked at conditions outside of PCOS. There were 16 articles that met final criteria and were included in this review. Results showed significant improvement in androgen and inflammatory markers but were inconsistent in anthropometric and blood sugar findings. Further studies with longer duration and increased generalizability are needed to more adequately compare probiotics to standard of care in the treatment of PCOS.
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.

